Your donation will support the student journalists of Bellaire High School. Your contribution will allow us to purchase equipment and cover our annual website hosting costs.
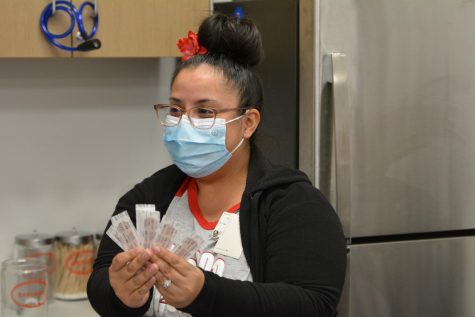
Nurse Chanthini Thomas calls the family of a confirmed positive student, asking questions about who they have come into contact with and if they have any siblings at home attending school. Thomas learned the correct process of contact tracing and other COVID prevention methods before the school year started, receiving certificates for her training as a school nurse.
An underequipped clinic’s fight against COVID: ‘It’s a wonder we have not died.’
COVID exposure may only be a chair away
Nov 8, 2021
A solitary chair sits in the hallway outside of room 1733, a small space that doubles as school nurse Chanthini Thomas’ clinic. Three air filters are placed throughout the room, bought by Thomas herself. Inside, she sets aside a stack of paperwork and briefly glances at the time before turning to the long list of emails that now await her. While she entered the clinic at 6 a.m., the clock now blinks 7:30 p.m. and Thomas is still hard at work.
Thomas’ current clinic is a temporary room, originally built to be a teachers’ lounge, meaning she lacks a proper isolation unit and has had to resort to creative measures. Over two months into the school year, the chair remains the sole method of quarantining for any students that come with symptoms.
“Suspected COVID-positive kids walk in and talk to us, so we’re exposed everyday,” Thomas said. “It’s a wonder we have not died. We’re constantly wiping, washing and cleaning.”
Thomas found herself preoccupied with local safety even before the pandemic-induced lockdown and recalled her initial reaction following the news about an infectious virus labeled COVID.
“I wasn’t paying attention to the news because my head was wrapped around safety and school,” Thomas said. “All of a sudden, Mr. Ngo [Magnet and AP Coordinator] told me that his trip to India might be canceled and mentioned ‘some virus going around.’ I come early and leave late, so I don’t see the news except in passing. I started paying attention, calling other nurses and Health and Medical Services.”
As the Committee Chairperson for Texas School Nurses Organization Region IV (TSNO) and member of the National Association of School Nurses, Thomas remained connected with an extensive network of fellow school nurses.
“People started sending me questions and our school nurse net was trying to figure out what was going on,” Thomas said. “All of a sudden, we get put out of school; that was March.”
Following the lockdown of in-person school in the 2019-2020 school year, HISD issued mandates for school nurses on top of their attempts to stay in contact with students with special medical needs.
“Students were more tech-savvy through their transition and everybody was worried about virtual school with teachers learning how to teach, but nobody taught the nurses and we weren’t aware of how to communicate, how to do anything,” Thomas said. “The district gave us mandates and said, ‘You must have at least 50,000 contacts with students and have to keep up with the kids.’ They were trying to make sure that kids stayed engaged.”
Around April of 2020, HISD invited Thomas to be on the District Communicable Disease Plan Task Force, a committee in charge of researching COVID-19 and creating a 134-page proposal of preventive measures for school called the HISD Communicable Disease Plan.
“That’s when we started doing nothing but research,” Thomas said. “We were all over CDC, WHO, other states and countries; we were just calling and sucking up every piece of information that we could.”
The committee presented their proposal – the HISD Communicable Disease Plan – to the former superintendent Grenita Lathan afterward. The proposal outlined how they thought the school year should be implemented, with the notes on the best mitigation methods like cleaning services and hand washing.
“It was kind of scary because you didn’t know what was happening and it was going so fast,” Thomas said.
After months of research, Thomas said she gained a whole new knowledge foundation based on research, and adds that it is constantly changing with different protocols and procedures.
“Everyday, people would ask me, ‘What do you think?’” Thomas said. “It was my responsibility to be as knowledgeable as I could. Parents would ask, students would ask, teachers would ask, so I had to know and I felt that it was important for me to have the most accurate and up-to-date information.”
As summer came around and staff started preparations for the 2020-21 hybrid school year, Thomas and the clinic’s clerk, Shirley Alfaro, were required to remain on campus anytime students were present in the building. They both ended up staying at school all summer with a turnout of about 100 or 200 kids.
However, with the majority of students choosing to learn virtually, nearly 15,000 students were missing by the lockdown school year in HISD alone. Thomas said she discovered these absences while making the district-ordered contacts to students.
“We found out that people’s families were affected, and kids stopped going to school because they had to work and support their families,” Thomas said.
Having to rely solely on poorly updated digital information, the unavailability of contacts rendered Thomas helpless in many cases where she was trying to locate or contact students.
“The information in the computer is old and nobody updates the phone numbers, addresses or emails,” Thomas said. “After the new superintendent came, we got another program with transferred information but lots of things were missing. Everything that we had health-wise no longer existed. People’s immunizations and information from their doctors like arthritis or seizures were all gone.”
Thomas added that this lack of accessible medical history was made worse by “people refusing to answer.”
“People who were in middle school like seventh or eighth grade are now here in high school and we’re finding everyday that somebody has asthma or needs medicine,” Thomas said. “Some students don’t bring their EpiPens, so we’re still trying to get what they need at the school. All of this was on top of trying to read and understand and learn what was happening, so it was always new.”
With the rise of COVID cases and deaths, media coverage on healthcare and frontline workers increased, gathering support and even resulting in Google’s logo thanking essential workers. However, this rising encouragement did not cover every field and left the workers with less visible risk unnoticed.
“You see it in the news all the time, the focus on the hospitals and their nurses, but they forget that school nurses are frontline to everybody that walks in and you don’t ever hear anything,” Thomas said. “If I worked in the hospital, I’d be in an ICU [Intensive Care Unit] with two or three patients. You’re here and you’ve got 3000 plus.”
Thomas explained how the nurse’s role in school changed compared to her earlier years of experience in healthcare.
“The reason you really have nurses is so that the kids who have chronic illnesses can now come to school,” Thomas said. “When I first started being a nurse years ago, kids who had seizures or asthma weren’t at school everyday or they missed a lot. But now that you have a nurse and you can get orders and you can get medicine and you get to monitor them, attendance should be better because you can stay in contact with their doctor and parent.”
The recent HISD mask mandate went into court, with the judge ruling a temporary restraining order on Governor Greg Abott’s mask mandate prohibition. Thomas explained that she must stay unbiased and non judgemental as a school nurse, even if her extensive research may contradict the opinions of students or parents.
“I can’t push my beliefs on anybody and I can only give you the information and facts I know,” Thomas said. “Every nurse said that even with COVID, there was no flu. This was because we were forcing people to wash their hands and wear masks. That ought to show that those are good mitigation techniques.”

Thomas worried about the increasingly lax restrictions with masks and social distancing around the school.
“How do I get the word out that it’s not a joke?” Thomas said. “Some students may have done okay after getting COVID, but we have kids here who are immunocompromised, have gone through chemotherapy and are allergic to components in the vaccine – making them unable to receive it.”
An essential contributor to Bellaire’s health and safety, Alfaro participates in the contact traces she and Thomas have to do in order to find possible COVID cases.
“We would ask parents about who their children were last with, when they eat lunch and when they remove their masks and the parents would respond: ‘I don’t have to tell you.’” Alfaro said. “The parents have been rude, yelling and hanging up the phone on us.”
This behavior is not unique to Bellaire, with numerous cases where parents are left frustrated by the school’s insistence on quarantining a possibly positive student.
The HISD Health and Medical Services have created an outline of procedural health guidelines for students and employees. The packet includes a list of COVID symptoms: cough, loss of taste or smell, runny nose, nausea, fever and more. Alfaro explained that what most don’t understand is that “if students show one of any of the symptoms, we have to call a parent and they have to go home.”
“The parents are getting mad at us, saying their children are fully vaccinated or have had COVID before, but that doesn’t mean they can’t get it again or don’t have a variant,” Alfaro said.
Through directly calling and interacting with parents, Thomas addresses the problem that arises when parents become dishonest and conceal information.
“They don’t tell you that they have siblings at other schools, and you want to then call the nurse at that other school but sure enough, sometimes they tell and sometimes they don’t,” Thomas said. “So then you’re setting another school up if you’re not honest.”
Thomas offered her recommendation for students who suspect they might have COVID.
“First thing: don’t come,” Thomas said. “You’re presumed positive if you have one or more symptoms. The thing about COVID is that it’s so different for everybody; somebody could have a headache, somebody else could have a runny nose and diarrhea and somebody else could actually have a fever and cough.”
As a susceptible person to COVID-19 herself, Thomas realizes the risks she and Alfaro face on a daily basis.
“We’re anxious and worried,” Thomas said. “Kids are coming in everyday, and we’re waiting on a few students’ results right now.”

